Every pulmonologist relies on spirometry. It is familiar, standardised, and deeply embedded in respiratory care. Yet many clinics now notice a recurring challenge. Some patients struggle to perform force-dependent breathing efforts. Some patients, in fact, even report symptoms that spirometry alone cannot fully explain.
This is where a Forced Oscillation Technique device begins to add value. It does not replace spirometry. Instead, it answers a different clinical question. It shows how the airways behave during quiet, natural breathing, when effort is no longer a limiting factor.
As these gaps become more visible in day-to-day practice, clinicians are rethinking how lung function is assessed. The question is no longer which test is better, but when each test is most informative. This is why understanding when to use spirometry, when to add oscillometry, and how both work together is becoming increasingly important in modern clinics. This article aims to help you answer just that!
What Is A Forced Oscillation Technique Device?
A Forced Oscillation Technique device is designed to assess airway mechanics while the patient breathes quietly.
- There is no deep inhalation.
- There is no forceful exhalation.
- The patient simply breathes normally through a mouthpiece.
During this calm breathing, the FOT device sends gentle pressure oscillations into the airways. These oscillations interact with the lungs and return information about resistance and elasticity. From this response, clinicians gain insight into how open, stiff, or reactive the airways truly are.
This is why oscillometry is often described as effort-independent. The results from the FOT device reflect lung behaviour, not patient technique. This difference matters a lot, especially for clinics managing children, elderly adults, or patients with fatigue or breathlessness. In these situations, a respiratory oscillometry device can reveal airway behaviour that spirometry may struggle to capture reliably.
How Does a Respiratory Oscillometry Device Work?
Instead of producing volume-based outputs like spirometry, a respiratory oscillometry device presents airway behaviour through resistance and reactance values measured across different frequencies. These measurements may look unfamiliar at first, but each one is designed to answer a specific clinical question.
Together, they help clinicians understand:
- Where airway resistance is originating
- How elastic or stiff the lung tissue is
- Whether changes are occurring in the central airways, the peripheral airways, or both
This frequency-based view is what allows oscillometry to reveal patterns that are not always visible with forced breathing tests. Each parameter, when read in context, adds another layer to the airway story and sets the stage for more precise interpretation.
Key Parameters You Will See on a Forced Oscillation Technique Report
Once oscillometry testing is complete, the next step is interpretation. A Forced Oscillation Technique report presents a small set of core parameters, each reflecting a specific mechanical behaviour of the airways during quiet breathing. Understanding what each parameter represents allows clinicians to read the report with clarity and apply the findings directly to clinical decisions.
Below is a practical breakdown of the most commonly used oscillometry parameters and how they are interpreted in everyday respiratory practice.
R5 (Resistance at 5 Hz)
R5 reflects total airway resistance. It captures resistance from both the larger central airways and the smaller peripheral airways together. When R5 is elevated, it signals that airflow is meeting increased opposition somewhere along the breathing pathway.
R20 (Resistance at 20 Hz)
R20 focuses primarily on the central airways. Changes here often point toward issues in the larger bronchial passages rather than the lung periphery.
R5–R20 (Small airway index)
The difference between R5 and R20 highlights small airway involvement. A wider gap suggests that resistance is coming from the deeper, peripheral airways. This is often affected early in asthma, COPD, or post-infectious states.
X5 (Reactance at 5 Hz)
X5 reflects how elastic the lungs are. More negative values indicate reduced elastic recoil or increased stiffness in lung tissue. This often appears before an obvious obstruction on spirometry.
AX (Area of reactance)
AX summarises overall reactance abnormality. Higher AX values suggest greater dysfunction in the peripheral airways and reduced ability of lung tissue to respond smoothly during breathing.
Fres (Resonant frequency)
Fres is the point where resistance and elasticity balance each other. When Fres shifts higher, it often signals worsening airway mechanics and increased stiffness within the respiratory system.
Taken together, these parameters allow a Forced Oscillation Technique device to map airway behaviour in a layered and effort-independent way. Instead of asking the lungs to perform, the respiratory oscillometry device observes how they function at rest. This is precisely where it adds value alongside spirometry, not by replacing it, but by revealing what forced breathing cannot always show.
Where FOT Adds Value Compared to Spirometry?
Spirometry remains a cornerstone of respiratory assessment. It is essential for diagnosing obstruction and tracking changes in FEV₁ over time. However, there are clinical situations where spirometry alone does not explain what the patient is experiencing. This is where a Forced Oscillation Technique device adds depth rather than duplication.
-
Early small airway involvement
Many patients report symptoms long before spirometry begins to change. Breathlessness, chest tightness, or exercise intolerance may appear while FEV₁ remains within normal limits. In these cases, the Forced Oscillation Technique device often detects early peripheral airway involvement through changes in R5–R20 and AX. These shifts help explain symptoms that spirometry may not yet capture.
-
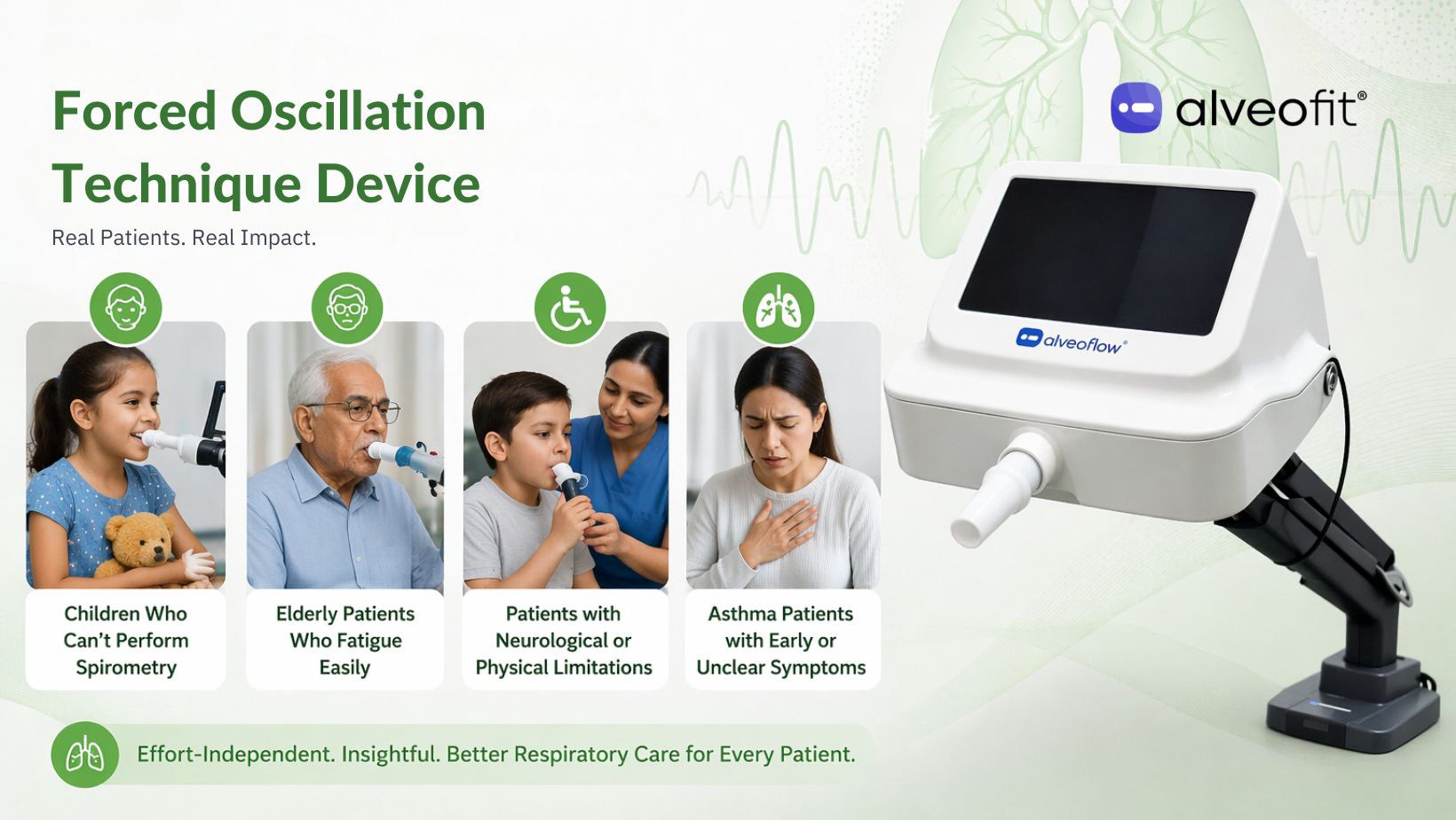
Children and older adults
Effort-dependent testing can be challenging for certain patient groups. Children may struggle with coordination, while older adults may fatigue quickly or fail repeated attempts. A respiratory oscillometry device allows airway assessment during quiet breathing. It reduces test failure and improves consistency without repeated coaching.
-
Understanding bronchodilator response more clearly
Some patients feel noticeably better after bronchodilator use, even when spirometry shows minimal change. A respiratory oscillometry device can reveal subtle reductions in airway resistance or improvements in reactance that align more closely with symptom relief. This added detail helps clinicians understand treatment response beyond forced flow measures.
-
Post-infectious and post-viral follow-up
After pneumonia or viral respiratory illness, patients often report lingering breathlessness despite acceptable spirometry results. Oscillometry can identify residual small airway dysfunction or increased stiffness during recovery, offering insight into why symptoms persist and how recovery is progressing.
Note: A Forced Oscillation Technique device does not replace spirometry in such situations. It actually complements it. Together, they provide a more complete and clinically meaningful picture of lung function.
Areas Where Spirometry Still Leads
A Forced Oscillation Technique device adds depth to lung assessment, but it does not replace every role spirometry plays. Some clinical questions still require effort-based testing.
- Volume and flow measurements still need spirometry: Values like FEV₁ and FVC can only be measured through forced breathing. These remain essential for diagnosis, staging disease severity, and following guideline-based care.
- Established standards and reference data favour spirometry: Spirometry has been validated over decades of clinical use. It is supported by broad normative datasets and well-defined diagnostic thresholds. These standards continue to anchor most respiratory guidelines and clinical frameworks.
- Certain reporting and protocol requirements rely on spirometric values: Many treatment pathways, audits, and documentation standards continue to be built around spirometry outcomes.
- Oscillometry requires informed interpretation: FOT results depend on factors such as posture, seal quality, and signal stability. However, clinicians are required to interpret patterns rather than rely on a single number.
In practice, clinics gain the most value by using both tools together. Spirometry answers effort-dependent questions. Respiratory oscillometry device, on the other hand, reveals airway behaviour at rest. Combined, they offer a more complete and clinically useful picture.
Conclusion
Spirometry continues to be a foundation of pulmonary assessment, but it does not answer every clinical question on its own. Some aspects of airway behaviour only become visible when effort is removed from testing. This is where a Forced Oscillation Technique device adds meaningful depth by revealing how the lungs behave during quiet, natural breathing.
The goal for pulmonology clinics is not to replace one test with another. It is to refine the assessment. When spirometry is combined with a respiratory oscillometry device, clinicians gain a more complete view of lung function, along with smoother testing and stronger clinical confidence.
As respiratory care becomes increasingly data-driven, clinics are beginning to adopt integrated solutions that bring both approaches together. alveofit offers advanced spirometry and a Digital Forced Oscillation Technique device for clinics. Our devices are designed to work in tandem and support clearer, more responsive respiratory assessment.
If you are looking to strengthen diagnostic clarity and future-proof your practice, exploring alveofit’s solutions is a practical next step.